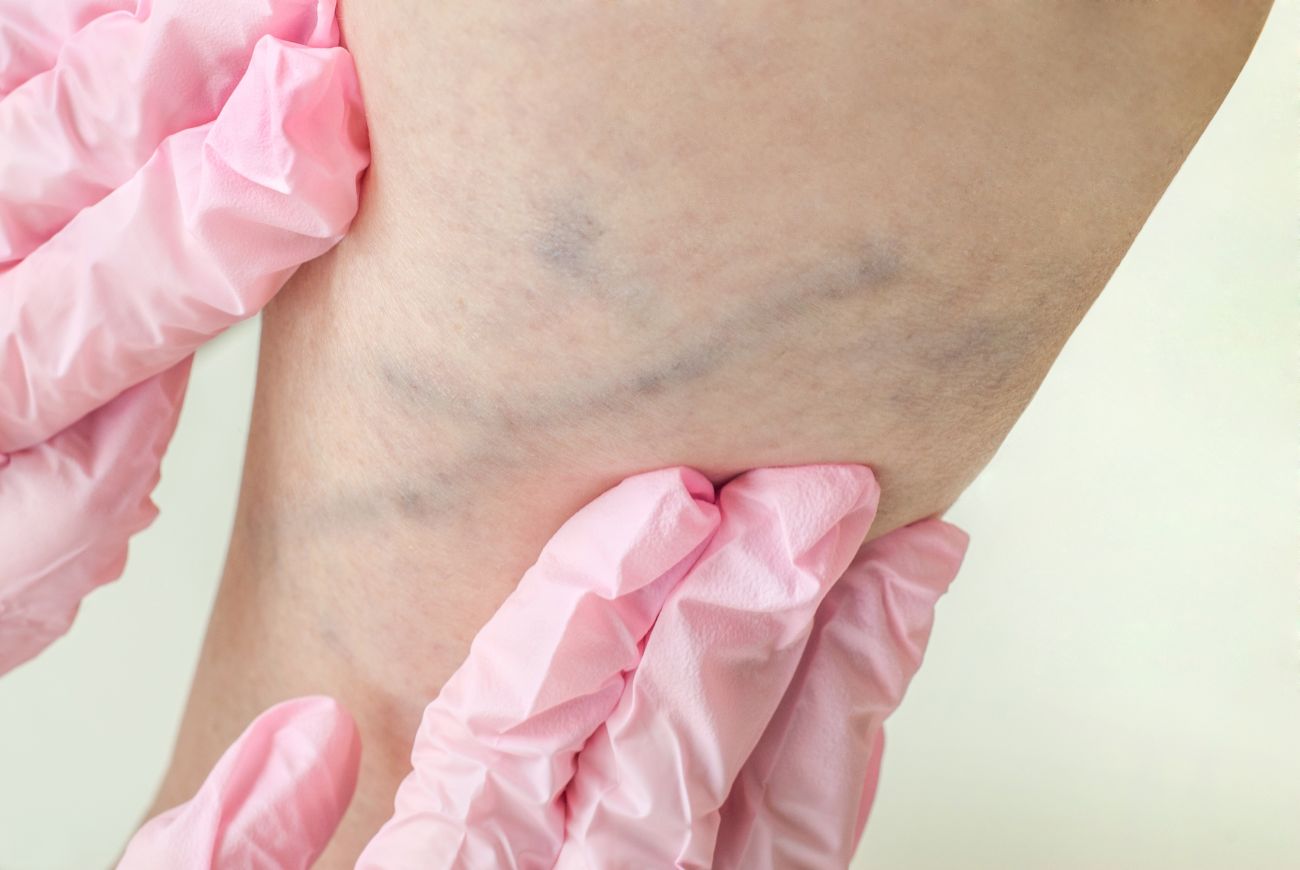
Do you know the warning signs of deep vein thrombosis? If not, familiarizing yourself with them could save your life someday.
Every year in the U.S., around 300,000 new cases of deep vein thrombosis, or DVT, are diagnosed. Given that the condition can easily progress into pulmonary embolism, which causes death around 30 percent of the time, knowing the warning signs is wise.
An initial bout of DVT can prompt an array of long-term issues. While pulmonary embolism is the most worrisome of the bunch, around one-third of those who develop DVT also develop post-thrombotic syndrome. This condition occurs due to permanent damage to the blood valves and vessels that has occurred due to a clot, which is also known as a thrombus.
Signs and Symptoms
The most common signs and symptoms of deep vein thrombosis include:
- Swelling in the affected area: DVT typically occurs in the legs. Oftentimes, the area of the leg around where the clot is located swells noticeably. This swelling tends to continue for as long as the clot is lodged in the vein, so any type of ongoing swelling is cause for concern.
- Pain: Due to the aforementioned swelling, the affected area may also be tender and painful. The pain may also originate from the clot that is lodged in the vein. At any rate, any ongoing pain, soreness, or tenderness that can’t be explained should be taken seriously.
- Redness or discoloration: Along with the symptoms that are mentioned above, the affected area that is near where the thrombus has developed may appear to be pink, red, or otherwise discolored. This again is primarily a result of the swelling that occurs due to the deep vein thrombosis. When accompanied by the other symptoms — especially swelling and pain — redness and discoloration are telltale signs of DVT.
- Warmth: The area around where the clot has formed in a deep vein may also feel warm to the touch. This has to do with the inflammation that goes along with DVT.
You may also not experience any outward signs of DVT. In that case, it may go undetected until a pulmonary embolism, or PE, occurs. With a PE, the clot that formed in the vein breaks free and travels through the bloodstream to the lungs. It then blocks one or more arteries where it can ultimately lead to death.
Some warning signs of PE that require immediate medical attention include:
- chest pain or discomfort that gets worse when you cough or take deep breaths
- sudden shortness of breath
- rapid pulse
- coughing up blood
- feeling dizzy or lightheaded, or fainting
Common Treatment Options
Treatment for DVT varies depending on several factors. A few of the most common treatments for deep vein thrombosis include:
- Blood thinners: Via either pills or injections, medications called anticoagulants, or blood thinners, are used to prevent clotting. Blood thinners won’t break up existing clots, but they prevent them from getting bigger and minimize the risk of new ones developing. Injected medications include heparin and fragmin; blood thinning pills that may be prescribed include warfarin and dabigatran.
- Clot busters: In severe cases, where a blood clot is at serious risk of trigger a pulmonary embolism, an IV line or catheter might be placed directly into the clot to break it up. This is known as thrombolytics.
- Filters: Another option to prevent the risk of life-threatening pulmonary embolism is to have a filter installed in the vena cava, which is the largest vein in the body. This filter works by preventing blood clots from making their way to the lungs.
- Compression stockings: For more mild cases of DVT that are deemed to be as likely to cause PE, compression stockings may be used to reduce swelling and to otherwise manage the condition. Many times, this option is enough to ward off the worst possible outcomes of the disease.
- Venous thrombectomy: This final option is the most invasive of them all, but it is also thankfully only required in very rare instances. If doctors determine that a blood clot is too large and at risk of breaking free, and if other methods won’t reliably prevent a pulmonary embolism, the clot in the deep vein may be cut out surgically.
Alternate Treatments
Most alternate treatments for deep vein thrombosis focus on making the blood thinner, which reduces the risk of clots forming. This can often be accomplished through dietary and lifestyle changes. Drinking at least six to eight eight-ounce glasses of water per day, for example, keeps the blood thinner and flowing more easily. According to studies from the University of Wisconsin, flavonoids that are found in red wine and grape juice help to trigger platelet production. In turn, this helps to keep the blood thinner and flowing.
Certain foods may also promote thinner blood. The phenols that are found in virgin olive oil, for example, may help to ward off clots. Garlic has long been prized for its ability to naturally thin the blood. In fact, people who take blood thinners are often warned to avoid it. Some patients are told to avoid leafy greens while on blood thinners because fluctuations in certain body chemicals can pose problems. Alternatively, you can be more consistent about consuming leafy greens.
Finally, it is highly recommended for anyone who is at risk for DVT to limit animal fats in their diets. In particular, saturated fats and trans fats should be kept at a minimum. Sugars should be avoided whenever possible too. Taking these steps reduces inflammation in the body, which in turn reduces the risk of blood clots forming in the deep veins.
Prognosis
While current treatment options for DVT are generally effective, they aren’t without their drawbacks. New treatments are being developed all the time. A few examples include:
- Mast cell inhibitors: In a study performed by researchers at the University of Birmingham in England and published in the journal Circulation Research, mice that were genetically depleted of mast cells, a type of immune cell, became protected from developing deep vein thrombosis. Mast cell inhibitors are a class of drugs that have long been used to treat allergic diseases like asthma, and these may prove effective in the treatment of DVT.
- NOACs: Over the last five years, the FDA has approved drugs that fall into a category called new oral anticoagulants, or NOACs. These promise to overcome many of the limitations of more common DVT treatments. In particular, they deliver more predictable effects, have a shorter half-life and require less monitoring. This means fewer trips to the doctor for patients, less bloodwork and a much easier time in general.
Now that you know the basics of DVT, be on the lookout for signs of the condition. Seek medical attention right away if you are worried that you have developed it.